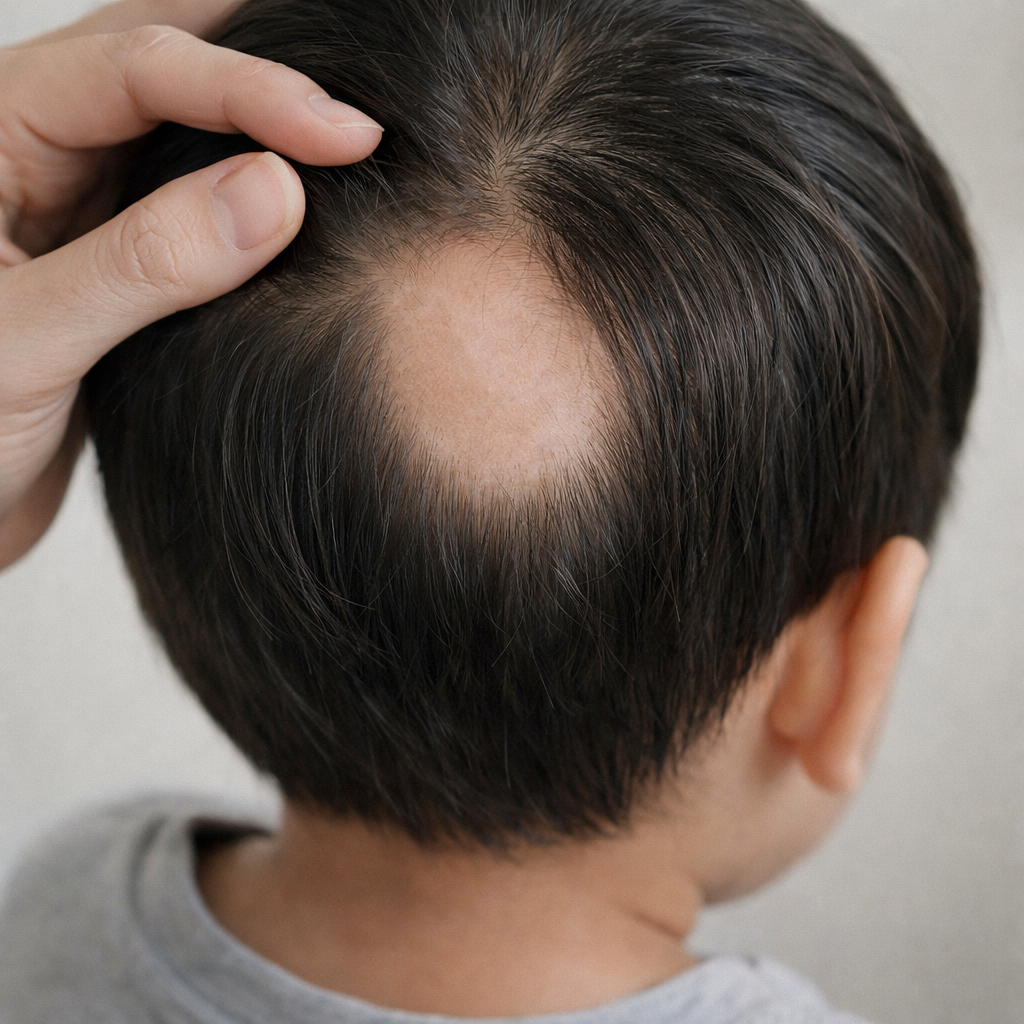
Hair loss in children: What triggers it? Causes parents should know…
Boy experiencing hair loss; patchy hair loss; parents checking their child's hair loss.
Common types of hair loss in children:
A variety of conditions can cause hair loss in children. Accurate identification is important for appropriate treatment and reassurance. Below are the most common types, their typical features and general approaches to management.
Alopecia areata
Cause: Autoimmune condition where the immune system attacks hair follicles.
Presentation: Well-demarcated, smooth, round or oval patches of hair loss. Can affect scalp, eyebrows and other body hair. In some cases progresses to total scalp hair loss (alopecia totalis) or whole-body hair loss (alopecia universalis).
Age: Can occur at any age, including childhood.
Diagnosis: Clinical examination; dermoscopy may show yellow dots, black dots and exclamation-mark hairs. Rarely need biopsy.
Management: Topical or intralesional corticosteroids (depending on age and size of patches), topical immunotherapy or topical minoxidil in some cases. Referral to a paediatric dermatologist or trichologist for persistent or extensive disease. Psychological support for the child and family is important.
Tinea capitis (scalp ringworm)
Cause: Fungal infection of the scalp (dermatophytes).
Presentation: Patchy hair loss with broken hairs, scaly or inflamed scalp; may form kerion (boggy, tender mass) in severe inflammatory cases. Often associated with itching and sometimes lymphadenopathy.
Age: Common in pre-school and school-age children.
Diagnosis: Clinical signs plus microscopy/culture or fungal PCR can confirm.
Management: Systemic antifungal therapy (oral griseofulvin or terbinafine depending on organism and age) is required; topical antifungal shampoos can reduce transmission. Prompt treatment prevents spread and scarring.
Telogen effluvium
Cause: Diffuse shedding triggered by a systemic stressor that causes an increased number of hairs to enter the telogen (resting) phase. Triggers include severe illness, high fever, surgery, nutritional deficiency or emotional stress.
Presentation: Diffuse thinning rather than patchy bald areas; usually noticed 2–3 months after the triggering event.
Age: Can occur in children after significant systemic stress.
Diagnosis: History of preceding stressor; hair pull test may be positive. Blood tests may be used to exclude nutritional deficiencies or thyroid disease.
Management: Identify and correct underlying cause (nutrition, treat illness, reduce stress). Reassurance: regrowth commonly occurs within months once trigger is removed.
Trichotillomania (hair-pulling disorder)
Cause: Repetitive hair pulling usually related to a behavioural or psychological condition.
Presentation: Irregularly shaped patches of hair loss with hairs of varying lengths and broken shafts. Scalp is typically not inflamed. Often localised to areas the child can reach.
Age: Often appears in school-age children and adolescents.
Diagnosis: Clinical history and pattern of hair loss; behavioural assessment may help.
Management: Behavioural therapies (habit reversal training, cognitive behavioural therapy), family support. Psychiatric or psychological referral as needed. Avoid punitive approaches.
Congenital and genetic hair disorders
Examples: Atrichia, hypotrichosis, certain ectodermal dysplasias.
Presentation: Hair may be sparse from birth or show abnormal growth pattern; other ectodermal structures (teeth, nails, sweat glands) may be affected in syndromic conditions.
Diagnosis: Clinical assessment, family history and genetic testing when indicated.
Management: Multidisciplinary approach with genetic counselling; symptomatic care and specialist referral.
Nutritional deficiencies
Cause: Inadequate intake or malabsorption of nutrients such as iron, zinc, biotin or essential fatty acids.
Presentation: Diffuse hair thinning rather than discrete patches; may accompany other signs like pallor or growth problems.
Diagnosis: Blood tests for iron studies, zinc, vitamin levels and overall nutritional assessment.
Management: Correct deficiencies through diet and supplementation under medical guidance.
Scarring (cicatricial) alopecia
Cause: Inflammatory or infectious conditions that destroy hair follicles leading to permanent hair loss.
Presentation: Hair loss with scalp scarring, loss of follicular openings, sometimes associated pain or recurrent infections.
Causes in children: Rare but may be due to severe infections, trauma, burns or rare inflammatory disorders.
Diagnosis: Clinical assessment and scalp biopsy may be required.
Management: Early specialist referral to try to halt progression; some scarring is irreversible so prevention and prompt treatment are crucial.
Alopecia Areata In Children
Overview Alopecia areata is an autoimmune condition that causes patchy hair loss. It can affect children of any age, from infants to adolescents. The condition most commonly presents as one or more smooth, round patches of hair loss on the scalp but can also involve eyebrows, eyelashes and body hair. Onset in childhood is common and may be associated with a higher risk of more extensive hair loss.
Causes and risk factors
Autoimmune reaction: The immune system mistakenly targets hair follicles, causing hair to fall out.
Genetics: A family history of alopecia areata or other autoimmune diseases (thyroid disease, vitiligo, type 1 diabetes) increases risk.
Triggers: Illness, emotional stress or minor skin trauma may precede episodes, though a direct cause is often not identified.
Age at onset: Younger children may have a more unpredictable course and a greater likelihood of progression to alopecia totalis (complete scalp loss) or universalis (complete body hair loss).
Symptoms and signs
Small, round, smooth patches of hair loss on the scalp.
“Exclamation mark” hairs: short hairs that taper at the base near the scalp.
Nail changes in some children: pitting, ridging or brittle nails.
Itching or tingling is uncommon but can occur before hair falls out.
Assessment and when to seek Hair specialist:
Take a careful history (onset, progression, associated symptoms, recent illness, family history, grooming habits).
Examine the scalp and hair with a Hair Specialist with experience in successful treatment and examination of Alopecia Areata in Children.